Overview:
Spinal Cord Stimulator Implant in Austin, TX
Physical pain is something most of us are familiar with and is part of our body’s healing process. Sometimes though, this pain lingers for months or even years.
Physical pain is something most of us are familiar with and is part of our body’s healing process. Sometimes though this pain lingers for months or even years.
This kind of ongoing pain is termed chronic pain. A recent study found that an estimated 20.4% (50 million) of U.S. adults had chronic pain, and 8.0% of U.S. adults (19.6 million) had high-impact chronic pain.1 The most common treatment options include medication, physical therapy, and cognitive behavioral therapy.
Sometimes, even after multiple treatment options have been explored, the pain does not subside. When all non-surgical treatments have failed, pain specialists recommend a special electrical stimulation therapy known as spinal cord stimulation or neurostimulation. This helps mask the pain or stimulate the nerves in the spine before the pain signals are sent to the brain.
Using a spinal cord stimulator
One of the most commonly recommended methods is the use of a spinal cord stimulator, predominantly because of its high success rate in reducing chronic pain conditions. A spinal cord stimulator (SCS or “neurostimulator”) is a small device that is surgically implanted under the skin. This implanted device sends mild electric currents to the spinal cord and stimulates the nerves in the area where pain is experienced. These electrical currents then mask or modify these pain signals before they reach the brain.
Benefitting from spinal cord stimulators
Use of spinal cord stimulator implant is most commonly recommended by medical practitioners for people who suffer from chronic pain of the back or limbs. It has been found to be successful in cases where patients have failed to get any relief even after surgeries or medical interventions. Here are several conditions where a spinal cord stimulator implantation is recommended:
- Pain from Nerve Damage
- Nerve-related pain (Diabetic neuropathy, etc.)
- Heart pain
- Spinal cord injuries of the neck, which can be treated with cervical spinal cord stimulation
- Peripheral vascular disease
- Complex regional pain syndrome
- Failed Back Surgery
- Arachnoiditis
This procedure is frequently used along with other pain management treatments such as medicines, exercise, and relaxation methods.
Working a spinal cord stimulator.
Before understanding the actual process of using a spinal cord stimulator, it is vital to get a broad overview of how it works and the components that go into making it a pain-relieving device.
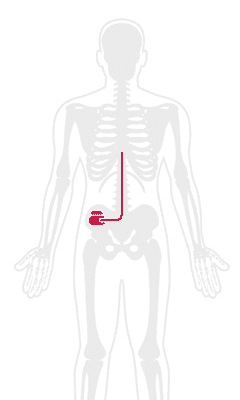
The spinal cord stimulator device is comprised of two parts: thin wires, or electrodes, and a generator, which is like a pacemaker. Between 8 and 32 electrodes are implanted in between the vertebrae and the spinal cord and the generator is placed just beneath the skin.
The patient has full control over the device. A remote control is provided to turn the device on or off, up or down. Usually the device remains on 24/7.
The device can replace pain sensations with a mild tingling called paresthesia. This is a pleasant sensation. Newer ones offer sub-perception stimulation to completely mask the pain, with no residual sensations. All types work with a remote control for the patient to manipulate the stimulation as required. Later models also have different waveforms for the electrical delivery – high frequency, high density, or burst stimulations.
Implanting the spinal cord stimulator
As a first step, your physician needs to determine if you are ready to receive spinal cord stimulation implantation. This is done via a series of imaging tests as well as a psychological evaluation, which gives the medical practitioner a holistic perspective on whether the device will function efficiently in your body.
After some imaging tests and psychological screening to see if the device is right for you, a neurosurgeon/pain specialist with specialized training in interventional pain management techniques performs the implantation procedure. There are two steps in the procedure for implanting the device:
- Initial Trial — Temporary electrodes are placed, and an external device is used to generate the electrical current. This procedure is done under x-ray guidance (fluoroscopy). The patient is usually asleep under anesthesia for this procedure. Afterwards, the patient goes home and resumes normal activity to “try out” the stimulator before committing to the implant.
- Implantation — Typically done as an outpatient procedure (approximately 1 hour), the generator is placed under the skin and the temporary electrodes are replaced with sterile electrodes that are anchored with sutures.
Post-surgery recovery
As it is an outpatient process, patients can go home once the effect of the anesthesia wears off. The device is programmed to suit your requirement, and you are sent home with a handheld remote control that allows the patient to turn it up or down, on or off.
Your physician will advise you to be very careful of your movement so that you do not pull at the incisions. Incisions usually heal between 2 and 4 weeks. Light activities such as moderate walking and driving is generally recommended the first two weeks. Complete recovery/return to normal life is usually around 6 to 8 weeks.
On follow-up visits, the physician may alter the settings of the pulse generator – the frequency of the pulses, the width of the area where the pulses are felt, and the amplitude that determines the threshold of the pain perception.
This surgery is a reversible process, which means that the neurostimulator can be removed without any repercussions to the spine or nerves, if there is no longer any need or desire for it.
Living with a spinal cord stimulator
Once your doctor feels that the process of post-surgery recovery is complete and your body is reacting to the implant well, you can go back to your normal routine.
Around 90% of patients successfully benefit from spinal stimulation, with up to 90% or more reduction in pain.
Most patients are able to stop or significantly reduce oral medication. If you have any doubts regarding specific activities, remember that it is always best to consult your physician first.
FAQS
Q: How does chronic pain escalate, requiring you to opt for immediate treatment?
A: Any external stimulus such as an injury or disease can cause mild to intense discomfort to our body. This sensation of discomfort is sent as signals via the nerves in the specific area to the brain, which identifies this sensation as pain.
Often, when medical interventions like pain medicines or opioid treatments fail to produce the desired results, the pain could escalate into a chronic pain condition. This means that the nerves continue to send constant signals to the brain, at times, even after the original injury that caused the pain has been treated.
Sometimes, the injury or medical condition could impair the nerves as well. As a result, pain signals could continue to be sent even if there is no injury to treat anymore. This constant transmission of pain signals could then also escalate into a chronic pain condition, leading to other physical and psychological conditions. It is essential to treat chronic pain through an appropriate pain management approach.
Q: Are there any side effects of using a spinal cord stimulator?
A: While complications are rare, patients may experience conditions such as infection, device migration, device damage, puncture to the dura matter around the spinal cord, epidural hematoma, epidural fibrosis, allergic reactions, and/or skin erosion.
Immediately call your doctor if you are experiencing any of the following: fever over 101.5° F, nausea, severe pain or signs of infection, rash or itching, numbness or weakness, visible swelling and/or loss of vital bowel/bladder functions.
Q: Can I have X-rays and CT scans with a spinal cord stimulator?
A: Certain types of tests or procedures may cause damage to the stimulator unless it is turned off during the process. Before you opt for any kind of procedure, ensure that you inform your healthcare provider that you have an implanted spinal cord stimulator device. For x-rays and CT scans, it is mandated that the device be switched off.
Q: Are spinal cord stimulators MRI compatible?
A: Before deciding on an MRI procedure, you should talk to your doctor. Several spinal cord stimulator devices in the market are not entirely compatible for an MRI while some will still enable you to undergo MRIs in specific regions.
If you have a spinal cord stimulator device that is not compatible for undergoing MRIs, it may cause some parts of the implant to get dislodged, overheat the device, or cause permanent damage to it. This may cause uncomfortable jolting or burning sensations in your body.
Q: What are some medical procedures that may affect my spinal cord stimulator device?
A: Before undergoing any medical test or procedure, it is critical that you inform your physician about your implanted device. There are some procedures or other devices that may cause moderate to severe damage to the device. They include: diathermy, cardiac pacemakers, lithotripsy, electrocautery, external defibrillation, radiation therapy, and ultrasound scanning.
Q: Will my spinal cord stimulator set off airport security?
A: When you walk through security scanners or come under a metal detector at airports, your spinal cord stimulator device may be detected. You will have an implant card to carry on airplane trips.
When you walk through security scanners or come under a metal detector at airports, your spinal cord stimulator device may be detected. You will have an implant card to carry on airplane trips.
Q: Can I drive with a spinal cord stimulator?
A: Yes, you can drive with a spinal cord stimulator on and activated.
Q: Can I swim with a spinal cord stimulator?
A: Showering, bathing, or swimming with a trial implantation is a strict no. These activities are okay to resume once a permanent device has been put in and the doctor has given a go ahead based on how the sutures have healed.
Q: What is the success rate of a spinal cord stimulator?
A: Up to 90% of patients will respond to the trial with pain relief up to 90% or more.
Patients with an implant typically enjoy at least a 70% permanent improvement in their lifestyles with reduced pain.
Q: Who is a candidate for spinal cord stimulator?
A: Failed back surgery and nerve damage are prime candidates. Patients with chronic pain in back and limbs, post-surgery pain, and other conditions such as heart pain, arachnoiditis, spinal cord injuries, nerve-related pain (Diabetic neuropathy, etc.), peripheral vascular disease, and complex regional pain syndrome can explore the option of getting a spinal cord stimulator.
Note that the doctor will conduct comprehensive psychological and imaging tests to determine if you are the right fit for the device.
Q: How long does spinal cord stimulator surgery take?
A: The surgery typically takes 1 hour and is performed under anesthesia. The procedure is done in two parts: placing of the lead/electrodes in the epidural space and placing of the pulse generator under the skin in the abdomen or buttocks region.
As the surgery is done as an outpatient procedure, the patient is normally sent home after the effect of the anesthesia wears off.
Q: What type of exercise can I engage in with a spinal cord stimulator?
A: Doctors normally permit very mild exercise in the form of walking the initial 2 weeks of recovery. Lifting of heavy weights (above 15 pounds), bending, twisting, jumping, climbing, and such activities are not allowed for the first 6 weeks. Whatever routine you decide to adopt, it should be strictly under the supervision of your physician.
Q: Is spinal cord stimulation safe?
A: The most common complication of spinal cord stimulators is the possibility of electrode migration. This can be either reprogrammed or may require surgical repositioning. Mild to moderate infections are also possible, and other complications could be fracture of the electrodes, failure of the pulse generator, cerebrospinal fluid leakage, and hematoma.
All such complications are minimized by the right selection of the candidate before the procedure and with regular follow-up visits after the surgery.
Q: How long does the battery last in a spinal cord stimulator?
A: If you have a device with a rechargeable battery, the device will last up to 10 years. Devices with a non-rechargeable battery may need to be surgically replaced after 2 to 5 years.
Is a spinal cord stimulator the best chronic pain care solution for you? Schedule an appointment with a pain care specialist to find out if spinal cord stimulation is for you.